August 31, 2012 report
Polymer coating allows nanoparticles to diffuse through the brain
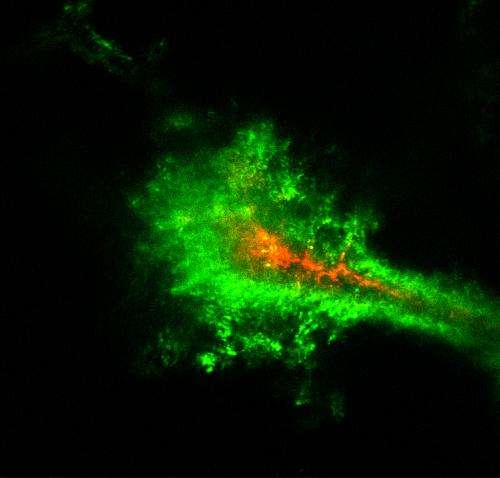
(Phys.org)—A new US study has found a way of enabling larger nanoparticles than previously to penetrate brain tissues, which may provide a new means of delivering therapeutic drugs to brain tissues for targeted treatment of conditions such as brain tumors and strokes.
A problem encountered when scientists have attempted to get nanoparticles into the brain is that the space between brain cells is sticky and too difficult for nanoparticles greater than 64 nanometers (nm) in diameter to get through. This limits the use of most nanoparticle drug delivery systems since the larger particles needed cannot effectively penetrate into the brain.
Researchers at Johns Hopkins University School of Medicine in Baltimore, led by Elizabeth Nance and Justin Hanes of the University's Department of Ophthalmology, experimented with nanoparticles of various sizes and coatings to try to find a way of enabling larger particles to diffuse within the brain.
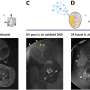
The problem, Hanes said, is that the extracellular brain fluid is "very sticky," with similar adhesive qualities to mucus, and this impedes the spread of particles larger than 64 nm in diameter. The solution the group found was to densely coat the particles with polyethylene glycol (PEG). They discovered that when coated, nanoparticles as large as 114 nm could diffuse within fresh ex-vivo human brains. The team confirmed the findings with particles up to 100 nm in the brains of living mice and dissected rat brains.
Polyethylene glycol is a low-toxicity polymer with a wide range of uses, including as a dispersant in toothpaste and skin creams, and as an anti-foaming agent in foods. As a coating for the nanoparticles, the PEG acts as a shield against hydrophobic and electrostatic interactions with the tissues and prevents the particles sticking to brain cells. At diameters over 114 nm, the particles begin to adhere, but Dr Hanes thinks the size limit could be as high as 200 nm.
The study's findings, published in Science Translational Medicine, may find application in more effective delivery of drugs to the brain tissues to treat conditions such as brain tumors, strokes and inflammation of the brain, but the researchers say that more research is needed on possible unwanted side effects or toxicity of drug-laden nanoparticles before clinical trials can begin.
More information: E. A. Nance, G. F. Woodworth, K. A. Sailor, T.-Y. Shih, Q. Xu, G. Swaminathan, D. Xiang, C. Eberhart, J. Hanes, A Dense Poly(Ethylene Glycol) Coating Improves Penetration of Large Polymeric Nanoparticles Within Brain Tissue. Sci. Transl. Med. 4, 149ra119 (2012). DOI: 10.1126/scitranslmed.3003594
Abstract
Prevailing opinion suggests that only substances up to 64 nm in diameter can move at appreciable rates through the brain extracellular space (ECS). This size range is large enough to allow diffusion of signaling molecules, nutrients, and metabolic waste products, but too small to allow efficient penetration of most particulate drug delivery systems and viruses carrying therapeutic genes, thereby limiting effectiveness of many potential therapies. We analyzed the movements of nanoparticles of various diameters and surface coatings within fresh human and rat brain tissue ex vivo and mouse brain in vivo. Nanoparticles as large as 114 nm in diameter diffused within the human and rat brain, but only if they were densely coated with poly(ethylene glycol) (PEG). Using these minimally adhesive PEG-coated particles, we estimated that human brain tissue ECS has some pores larger than 200 nm and that more than one-quarter of all pores are ≥100 nm. These findings were confirmed in vivo in mice, where 40- and 100-nm, but not 200-nm, nanoparticles spread rapidly within brain tissue, only if densely coated with PEG. Similar results were observed in rat brain tissue with paclitaxel-loaded biodegradable nanoparticles of similar size (85 nm) and surface properties. The ability to achieve brain penetration with larger nanoparticles is expected to allow more uniform, longer-lasting, and effective delivery of drugs within the brain, and may find use in the treatment of brain tumors, stroke, neuroinflammation, and other brain diseases where the blood-brain barrier is compromised or where local delivery strategies are feasible.
Journal information: Science Translational Medicine
© 2012 Phys.org